Learn how AI in medical billing is helping US providers reduce claim denials, automate RCM, and recover millions. Free billing audit from Malakos Healthcare Solutions.
Every year, US healthcare providers lose an estimated $262 billion to claim denials — not because they delivered poor care, but because of billing errors, outdated workflows, and a system that rewards complexity over clarity.
For clinic owners and practice managers, a high denial rate isn’t just frustrating — it’s a cash flow crisis. Staff spend hours reworking claims, chasing insurers, and resubmitting paperwork that could have been accurate the first time. The administrative burden is unsustainable.
That’s why artificial intelligence is no longer a buzzword in healthcare — it’s becoming the backbone of modern healthcare revenue cycle management. In this guide, we’ll break down exactly how AI in medical billing is transforming denial management, and what it means for your practice in 2026.
What Are Claim Denials?
A claim denial occurs when a health insurance payer refuses to reimburse a provider for services rendered. It is one of the most common — and costly — problems in healthcare billing today.
Soft vs. Hard Denials
- Soft denials are temporary rejections that can be corrected and resubmitted — for example, missing prior authorization or an incorrect date of service.
- Hard denials are final. Claims denied due to non-covered services, timely filing lapses, or fraud flags typically cannot be appealed and result in permanent revenue loss.
Why Do Denials Happen?
- Incorrect or missing patient information
- Coding errors (wrong ICD-10, CPT, or modifier codes)
- Prior authorization failures
- Duplicate claim submissions
- Eligibility verification gaps
- Late submissions beyond payer deadlines
- Coordination of benefits issues

The Challenges of Traditional Medical Billing
For decades, medical billing relied almost entirely on manual processes — human coders, paper trails, and spreadsheets. The results speak for themselves.

The result? Average denial rates between 15–20% across US healthcare practices — with some specialties seeing rates as high as 30%. This is not sustainable. And it is exactly the problem AI was built to solve.
What is AI in Medical Billing?
Artificial intelligence in the billing context refers to software systems that use machine learning, natural language processing, and predictive analytics to automate and optimize the entire claims lifecycle — from patient intake to final reimbursement.
Unlike traditional billing software that simply processes data you enter, AI learns from patterns. It can analyze thousands of historical claims, identify what caused denials, and proactively correct issues before a claim ever leaves your system.
Think of it as having a senior billing expert reviewing every claim — 24 hours a day, at unlimited scale, with zero fatigue and no sick days.
How AI Reduces Claim Denials — In Detail
Understanding how medical billing automation works in practice is key to appreciating its impact. Here are the six core mechanisms driving denial reduction:


Benefits of AI in Healthcare Revenue Cycle Management
The business case for adopting RCM solutions powered by AI is compelling. Here is what practices are experiencing:
Dramatically Reduced Claim Denials
AI-driven clean claim rates can exceed 96%, compared to the industry average of 75–80%. That is a direct, measurable impact on your bottom line.
Faster Reimbursements
Cleaner claims process faster. Practices using medical billing automation report reimbursement cycles shrinking from 45 days to under 15 — freeing up working capital.
Improved Cash Flow
Fewer denials and faster payments mean steadier, more predictable revenue — critical for small and mid-size practices managing tight margins.
Reduced Administrative Burden
Automation frees billing staff from rework. Teams can focus on complex cases, patient communication, and higher-value revenue cycle tasks.
Significant Cost Savings
The cost of reworking a denied claim averages $25–$118. AI-powered prevention is far cheaper than manual correction at scale — and the savings compound over time.
Real-World Use Cases: AI Billing in Action
The numbers are compelling — but what does improve claim accuracy look like on the ground? Here are representative examples of what AI-powered billing delivers:
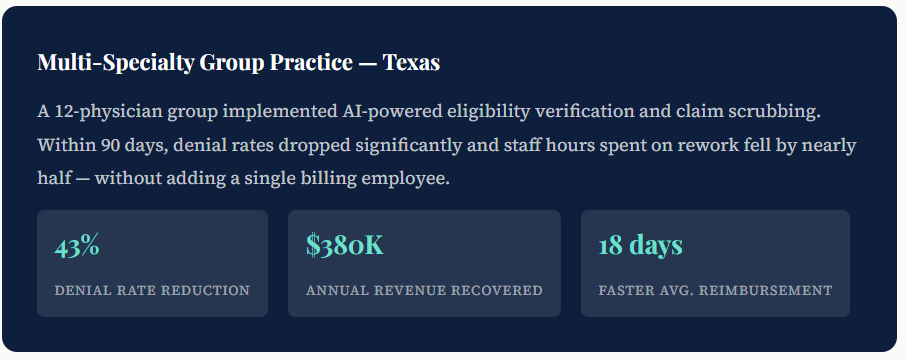
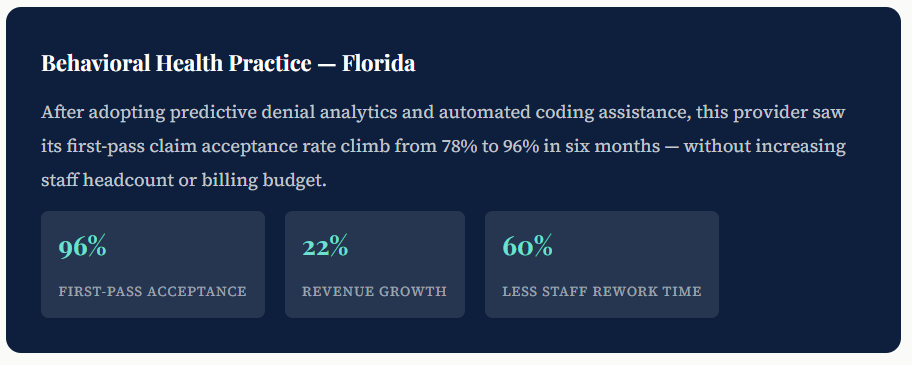
Challenges of AI Adoption in Billing
AI adoption is not without its hurdles. Healthcare providers considering new RCM solutions should be prepared for the following:
- Upfront investment: AI billing platforms require initial setup costs, though ROI typically materializes within 6–12 months for most practices.
- Staff training: Teams need time to learn new workflows and build confidence in AI-driven recommendations — change management matters.
- EHR integration complexity: Compatibility with existing electronic health records systems can be challenging without an experienced implementation partner guiding the process.

The Future of AI in Healthcare Billing — 2026 and Beyond
The trajectory is clear. AI in medical billing is moving from “nice to have” to mission-critical infrastructure for every US healthcare provider. Here is what is coming:
- Autonomous claims processing: By 2027, analysts project that over 50% of routine claims will be fully processed from documentation to reimbursement with no human involvement required.
- AI-powered appeals: Natural language AI will draft appeal letters, identify denial patterns across payer networks, and recommend appeal strategies — automatically.
- Predictive revenue forecasting: Practices will use AI to project monthly revenue with 95%+ accuracy, enabling smarter financial planning and staffing decisions.
- Payer-agnostic learning models: AI systems will continuously learn from denial data across hundreds of payers, making every claim sharper and more accurate than the last.
The practices that invest in improve claim accuracy infrastructure today will be the ones winning reimbursements — and market share — well into the next decade.
Conclusion
Claim denials are costing US healthcare providers hundreds of billions of dollars every year — and the majority are entirely preventable. The era of relying on manual billing processes, reactive denial management, and disconnected systems is ending.
AI in medical billing is not a futuristic concept. It is available today, proven in practices across the country, and delivering measurable returns within weeks of implementation. From automated claim validation to predictive denial analytics, the tools exist to transform your revenue cycle — right now.
The question is not whether your practice should adopt AI-powered billing. The question is how much revenue you can afford to lose while you wait.
Frequently Asked Questions
1. How much can AI actually reduce claim denials in my practice?
Real-world implementations show that AI-powered billing can reduce claim denials by 40–67% depending on specialty and current denial rate. Practices with high manual error rates typically see the fastest improvements — often within the first 60–90 days of implementation.
2. Is AI-powered medical billing affordable for small practices?
Yes. Many AI-integrated RCM solutions — including Malakos Healthcare Solutions — operate on a percentage-of-collections model, meaning you pay only when you get paid. This eliminates large upfront costs and aligns the billing company’s incentives directly with your revenue growth.
3. What types of claim denials can AI prevent most effectively?
AI is most effective at preventing eligibility-related denials, coding errors (incorrect ICD-10 or CPT codes), duplicate claims, missing prior authorizations, and timely filing failures. These categories account for the vast majority of all preventable denials in medical billing.
4. How does AI integrate with my existing EHR system?
Most modern AI billing platforms integrate with leading EHR systems including Epic, Athenahealth, eClinicalWorks, and others via HL7/FHIR APIs. Malakos Healthcare Solutions manages the full integration process, minimizing disruption to your existing clinical and administrative workflows.
5. How long does it take to see results from AI-powered billing?
Most practices begin seeing measurable improvements in first-pass acceptance rates and overall denial rates within the first 30–60 days. Full optimization — including the predictive analytics learning from your payer-specific data patterns — typically matures over 3–6 months of continuous operation.
© 2026 Malakos Healthcare Solutions. All rights reserved. This content is for informational purposes for US healthcare providers. Statistics referenced from AMA, HFMA, MGMA, and industry research reports.
Struggling with Family Medicine billing errors? Contact our team today for a free billing audit and improve your collections.







