Discover the top reasons family medicine billing claims get denied in 2026 and learn proven strategies to fix them fast, reduce revenue loss, and improve cash flow.
Introduction
Family medicine clinics are the backbone of American healthcare. Your providers see dozens of patients every day — routine checkups, chronic disease management, urgent visits, preventive care. The clinical side runs like clockwork. But behind the scenes, the billing side tells a very different story.
For many primary care practices, claim denials are a slow leak draining thousands of dollars every month. A wrong modifier here, a missed authorization there, and suddenly you’re chasing payments that should have arrived weeks ago. Staff are overwhelmed, resubmissions pile up, and revenue that belongs to your practice disappears into the system.
If your family medicine clinic is losing money to billing errors — you’re not alone, and more importantly, it doesn’t have to stay that way.
Common Challenges in Family Medicine Billing
Family medicine billing is uniquely complex. Unlike specialty practices that deal with a narrow set of procedures, primary care handles an enormous variety of visit types, diagnoses, and payers — all at high volume.
High Patient Volume and Documentation Errors
When a provider sees 25–30 patients a day, documentation shortcuts happen. Notes get delayed. Important clinical details don’t make it into the chart. Incomplete documentation is one of the most common triggers for claim denials because insurers need proof that the billed service was medically necessary and properly documented.
E/M Coding Confusion: 99213 vs. 99214
This is one of the most frequently misused areas in family medicine billing. Many practices default to 99213 for nearly every visit — either out of habit or to avoid scrutiny — even when the encounter genuinely qualifies as a 99214. Others go the other way and overcoded, which triggers audits. Since 2021, E/M coding has been based on medical decision-making (MDM) or total time, but many smaller practices haven’t fully updated their workflows to reflect this.
Undercoding means leaving real money on the table. Overcoding means audit risk. Getting it right requires consistent training and documentation standards.
Preventive vs. Problem-Based Visit Billing
A patient comes in for their annual wellness visit and mentions their knee has been hurting. The provider addresses it. Now you have two separate billable services — a preventive exam (99395–99397) and a problem-based E/M visit (99213–99215) — each with its own coding and modifier requirements.
Many practices either miss the second charge entirely or bill it incorrectly, resulting in denials or lost revenue.
Insurance Verification and Eligibility Issues
Billing a claim to an inactive plan or wrong payer is an instant denial. In family medicine, patients often have insurance changes tied to life events — new employment, Medicaid eligibility shifts, Medicare crossovers — and practices don’t always catch these before the visit.
Frequent Claim Denials and Underpayments
Even when claims go out clean, denials still happen. Coordination of benefits errors, timely filing issues, and missing authorizations account for a significant share of denials that practices often write off rather than fight. That’s money left uncollected.
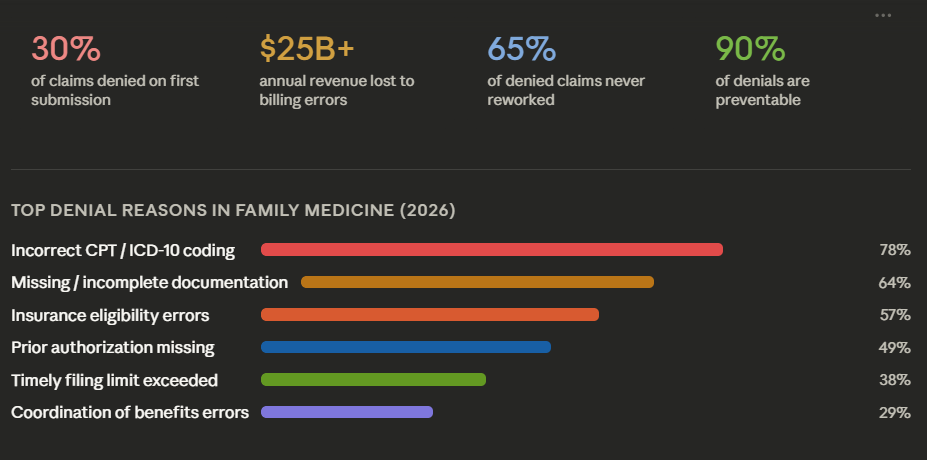
Top Reasons Claims Get Denied in Family Medicine in 2026
Understanding why denials happen is the first step to preventing them. Here are the most common culprits in 2026:
Incorrect CPT or ICD-10 Coding A mismatched diagnosis code, an outdated CPT code, or a missing modifier can cause an immediate rejection. Payer systems flag these automatically, and they rarely give the benefit of the doubt.
Missing or Incomplete Documentation Insurers deny claims when the medical record doesn’t support the level of service billed. If the chart doesn’t tell the story, the claim won’t get paid — it’s that simple.
Prior Authorization Issues Certain procedures, referrals, and diagnostic tests require pre-approval. Submitting without it — or with the wrong authorization number — results in immediate denial. Payer auth requirements change frequently, and keeping up is a full-time job in itself.
Timely Filing Limits Most payers have strict deadlines: 90 days, 6 months, or 12 months from the date of service. Claims submitted after the deadline are denied with no right to appeal in most cases. A backlogged billing team misses these windows more often than practices realize.
Coordination of Benefits (COB) Errors When a patient has more than one insurance plan, the primary and secondary payers must be billed in the right order. A COB error means one or both payers deny the claim — and the practice gets stuck chasing a resolution that takes weeks.
How to Fix These Issues: Practical Solutions for Your Practice
The good news is that most denials are preventable. Here’s what high-performing family medicine practices are doing differently:
Build a Consistent Documentation Workflow Create standardized note templates that prompt providers to include the key elements payers look for — chief complaint, history, MDM rationale, and plan. Require providers to complete and sign notes the same day.
Train Staff Regularly on Coding Updates Coding guidelines change every year. Set up quarterly training sessions for front desk, clinical, and billing staff. Make sure everyone understands the difference between preventive and E/M billing, and how to use modifiers correctly.
Verify Eligibility Before Every Visit Don’t rely on existing records. Run eligibility checks 24–48 hours before each scheduled appointment and again on the day of service. Most practice management systems have real-time eligibility tools — use them.
Set Up a Denial Tracking System Log every denial, the reason, and the outcome. Over time, you’ll see patterns — specific payers, specific codes, specific providers — that tell you exactly where to focus your prevention efforts.
Work With an Experienced Billing Partner If your in-house team is stretched thin, outsourcing to a specialized medical billing partner for family practice means you get certified coders, denial management expertise, and consistent follow-up — without the overhead of hiring and training additional staff.
Why Outsourcing Family Medicine Billing Makes a Real Difference
More and more primary care practices are turning to RCM partners for family medicine — and for good reason.
When your billing is handled by specialists who understand the nuances of family practice coding, you see faster reimbursements, fewer denials, and a cleaner AR. Your team can focus on patient care instead of chasing payments. And your practice has better visibility into its financial performance through regular reporting and benchmarking.
A good billing partner doesn’t just submit claims — they manage your entire revenue cycle, from eligibility verification through payment posting and denial resolution.
Get a Free Billing Audit from Malakos Healthcare Solutions
If your family medicine clinic is dealing with high denial rates, slow reimbursements, or revenue you just can’t account for — it’s time to find out exactly what’s happening.
Malakos Healthcare Solutions specializes in family medicine billing services for primary care practices across the United States. We handle the complexity so you can focus on your patients.
Schedule your free billing audit today. We’ll review your current denial rates, coding patterns, and revenue cycle performance — and show you exactly where you’re losing money and how to get it back.
[Contact Malakos Healthcare Solutions] | [Request Your Free Audit]
Conclusion
Claim denials in family medicine billing aren’t just a billing department problem — they’re a practice-wide revenue problem. From coding confusion and documentation gaps to eligibility errors and missed authorization requirements, the causes are many but the solutions are clear.
The practices that get this right share a few things in common: strong documentation workflows, up-to-date coding knowledge, proactive eligibility verification, and a billing partner who knows how to fight for every dollar. In 2026, with payer requirements growing more complex by the year, having the right billing support isn’t a luxury — it’s a competitive advantage.
Your revenue should work as hard as your team does. Let’s make sure it does.
Your work matters. Make sure you’re getting paid for it.
Malakos Healthcare Solutions — Billing Expertise for Integrative Healthcare Providers
📞 +1 307-441-3431 | 📧 support@malakoshcs.com







