For too many chiropractic practices across the United States, consistent revenue doesn’t hinge on patient volume it hinges on what happens after the patient walks out the door.
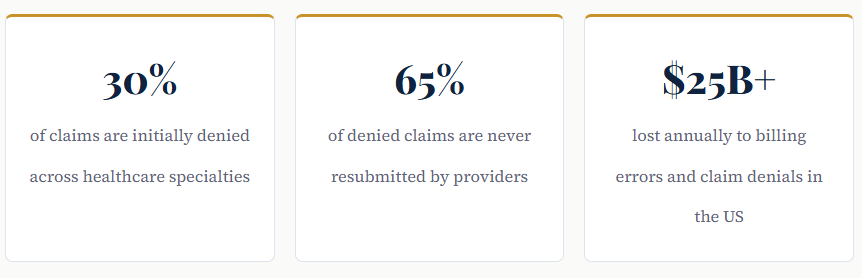
Claim denials are one of the most persistent and costly problems facing chiropractic clinics today. According to industry estimates, healthcare providers lose billions of dollars each year to denied or delayed claims and chiropractic offices are disproportionately affected due to the complexity of payer rules surrounding spinal manipulation and manual therapy codes. The root cause, in the vast majority of cases, comes down to avoidable chiropractic billing mistakes that slip through during the coding, documentation, or submission process.
If your clinic is seeing a growing pile of denied claims, delayed reimbursements, or unexplained write-offs, chances are that one or more of the billing errors described in this article are quietly draining your revenue. The good news: every one of them is fixable.
Common Chiropractic Billing Mistakes That Trigger Denials
Not all billing errors look alike. Some are subtle a missing modifier on a claim line while others are systemic, reflecting deeper gaps in workflow or training. Here are the most frequent chiropractic billing mistakes that result in claim denials:
Incorrect CPT Code Selection
Chiropractic spinal manipulation codes (98940–98943) are defined by the number of spinal regions treated. Billing the wrong CPT code — even by one region — gives payers grounds for denial or downcoding. Similarly, using outdated codes or failing to differentiate between chiropractic manipulative treatment (CMT) codes and physical medicine codes creates frequent mismatches with payer fee schedules.
Missing or Incorrect Modifiers
Modifiers communicate critical context to payers — whether a service was performed by the billing provider, whether it’s a distinct procedure, or whether medical necessity applies. Omitting modifiers like AT (active/corrective treatment) on Medicare claims, or misapplying modifiers on combination service visits, is one of the leading causes of automatic claim rejection in chiropractic offices nationwide.
Documentation Errors and Gaps
Payers require clinical documentation that supports every billed service. SOAP notes that lack specificity — failing to document subjective complaints, objective findings, a clear assessment, and a measurable treatment plan — give insurers justification to deny claims for lack of medical necessity. Incomplete or copy-pasted notes are a red flag during audits and a direct path to revenue loss.
Insurance Verification Failures
Submitting a claim before verifying a patient’s active coverage, chiropractic benefits, visit limitations, and referral or authorization requirements is a guaranteed path to denial. Coverage details change at plan renewal, after employment changes, and at the start of each calendar year — making front-desk verification a non-negotiable step before every patient encounter.
Why These Billing Mistakes Keep Happening
Lack of Specialized Billing Expertise
Chiropractic billing is not general medical billing. It operates within a unique set of payer rules, coverage limitations, and coding nuances. Many clinics rely on staff who are competent generalists but haven’t received chiropractic-specific training in CPT coding, modifier usage, or Medicare compliance. Without that specialized foundation, even well-intentioned billing teams will produce errors.
Overloaded In-House Staff
In smaller practices, billing responsibilities often fall on the same staff handling front-desk duties, scheduling, and patient intake. When billing is one task among many rather than a dedicated function, errors accumulate. Claims are submitted without thorough review, denial follow-up is deprioritized, and the accounts receivable backlog quietly grows.
Key insight: Most chiropractic billing mistakes aren’t caused by carelessness — they’re caused by systemic gaps in training, workflow, and dedicated oversight. Fixing the system is more effective than fixing individual errors one at a time.
The Real Impact on Your Clinic’s Revenue
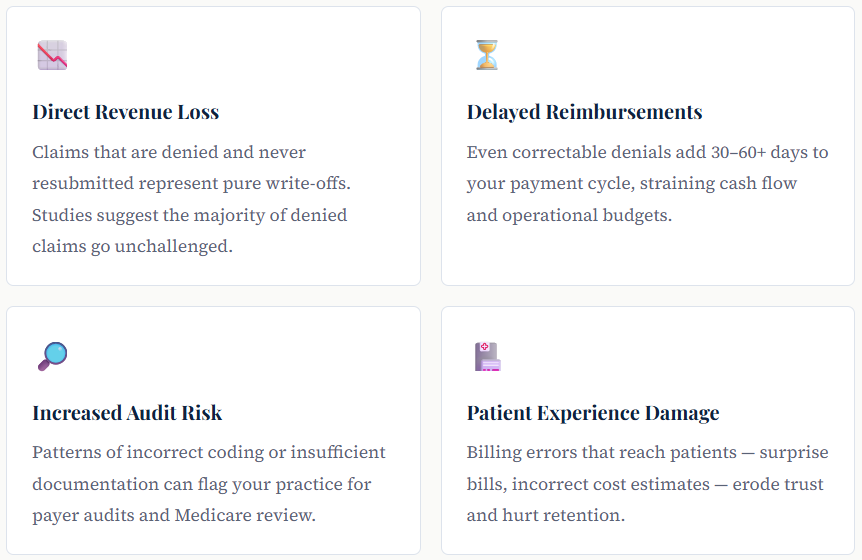
The financial consequences of persistent chiropractic billing mistakes extend far beyond a single denied claim. When errors are systemic, the damage compounds over time:
How to Fix These Chiropractic Billing Mistakes
Implement Rigorous Coding Protocols
Every clinician should document the number of spinal regions treated in a way that directly maps to the correct CPT code before the claim is ever touched by billing staff. Creating a clear internal crosswalk between clinical documentation and CPT selection reduces ambiguity and downstream errors significantly.
Build a Pre-Submission Documentation Checklist
Before any claim leaves the practice, a checklist review should confirm that SOAP notes are complete, medical necessity is clearly supported, modifiers are applied correctly, and the diagnosis codes (ICD-10) link logically to the billed procedures. A 10-minute pre-submission review can prevent weeks of denial follow-up.
Establish a Proactive Denial Management Process
Denials should be tracked, categorized by reason code, and analyzed monthly to identify patterns. If the same CPT code is being denied repeatedly by the same payer, that’s a signal to investigate payer-specific policy, not just resubmit the claim. A structured denial management workflow ensures revenue isn’t simply abandoned.
Invest in Ongoing Staff Education
Chiropractic coding guidelines are updated annually. Allocating time and budget for regular training — whether through AAPC resources, payer-specific webinars, or in-house audits — keeps your billing team current and reduces error rates over time.
The Case for Outsourcing Chiropractic Billing
For many practices, the most effective solution to recurring chiropractic billing mistakes isn’t hiring more staff or purchasing new software — it’s outsourcing to a specialized chiropractic billing service.
Fewer Errors, Higher Clean Claim Rates
Dedicated chiropractic billing companies employ coders and billing specialists whose entire focus is chiropractic revenue cycle management. Their familiarity with payer rules, modifier requirements, and documentation standards translates directly into higher first-pass claim acceptance rates — often above 95% in well-run operations, compared to industry averages in the low-to-mid 80s for in-house teams.
Faster Reimbursements and Healthier Cash Flow
When claims are submitted correctly the first time, the payment cycle shortens dramatically. Outsourced billing teams also actively follow up on outstanding claims and manage the full denial lifecycle — meaning less money left on the table and a more predictable monthly revenue stream for your clinic.
- Expertise in chiropractic-specific CPT and ICD-10 coding
- Dedicated Medicare and commercial payer compliance oversight
- Systematic denial tracking and appeals management
- Regular reporting and KPI visibility for clinic owners
- Reduced administrative burden on clinical and front-desk staff
Conclusion
Claim denials are not an inevitable cost of doing business in chiropractic care. In the vast majority of cases, they are the predictable result of specific, correctable chiropractic billing mistakes — incorrect codes, missing modifiers, documentation gaps, and verification failures that compound silently until they become a serious revenue problem.
Whether you choose to invest in internal process improvements, staff training, or a trusted billing partner, the most important step is acknowledging that billing accuracy is a clinical and business priority — not an afterthought. Your patients deserve exceptional care. Your practice deserves to be paid for it.
Let’s Fix Your Billing — Starting Today
Struggling with chiropractic billing errors? Contact our team today for a free billing audit. We’ll identify exactly where your claims are falling through the cracks and outline a clear path to fewer denials and faster reimbursements.

