Reduce AR days with proven strategies to improve cash flow, reduce denials, and speed up payments in healthcare billing.
If you run a medical practice whether it’s a solo clinic or a multi-physician group there’s one number that quietly makes or breaks your financial health: your AR days. Learning how to reduce AR days in healthcare isn’t just an accounting exercise. It directly affects whether you can pay your staff on time, invest in better equipment, and keep your doors open.
Let’s be real: most providers go into medicine to help patients, not to chase insurance companies for money. But the reality is that slow, unpaid claims add up fast. When your accounts receivable starts aging, it doesn’t just affect cash flow it creates a domino effect of operational headaches.
In this guide, we’re breaking down exactly what AR days are, why high AR days hurt your practice, and most importantly the specific, practical steps you can take right now to get paid faster.
What Are Reduce AR Days in Healthcare?
AR days short for Accounts Receivable Days measure how long it takes your practice to collect payment after a service is delivered. In simple terms: from the moment you see a patient to the moment you actually receive the money, how many days does it take?
AR Days = (Total AR Balance ÷ Average Daily Charges)
Example: $150,000 AR ÷ $5,000 avg. daily charges = 30 AR Days
The lower the number, the faster you’re getting paid. Most industry experts agree that a well-run practice should aim for an AR days benchmark of 30–40 days or fewer. If your AR days are creeping past 50 or 60, that’s a warning sign something in your medical billing process needs attention.
Why High AR Days Are a Problem for Your Practice
Think of accounts receivable in healthcare like water in a pipe. When it flows freely, everything works. When it gets clogged, pressure builds — and things start breaking down.
Here’s what actually happens when your AR days start climbing:
- Revenue gets stuck. You’ve delivered the care, but the money hasn’t arrived yet. That means payroll, supplies, and rent all come out of a shrinking pool of cash on hand.
- Old claims are harder to collect. Claims that go unpaid past 90–120 days become significantly harder to recover. Insurers may deny them outright or require extensive documentation.
- Staff burnout increases. Constantly chasing down denials and resubmitting claims is exhausting. High AR days often mean your billing team is stuck in reactive mode instead of proactive.
- It masks bigger billing problems. Rising AR days are often a symptom of deeper issues — coding errors, eligibility failures, or weak denial management protocols.
- Your cash flow suffers. Practices with high AR days often can’t reinvest in growth — new hires, technology upgrades, or expanded services.
Quick Stat: According to the American Medical Association, physician practices spend an average of $99,000 per physician annually just on prior authorization and billing administrative work and that number rises when AR days are poorly managed.
Top Causes of High AR Days in Medical Billing
Before you can fix the problem, you need to understand what’s causing it. In our experience working with healthcare practices across the US, these are the most common culprits:
- Billing errors and data entry mistakes. A wrong date of service, an incorrect patient ID, or a missing modifier can cause an instant rejection.
- Insurance eligibility not verified upfront. Submitting a claim only to find out the patient wasn’t covered on that date? That’s a completely avoidable AR day killer.
- Poor or slow follow-up on unpaid claims. Many practices don’t have a consistent process for tracking aging claims and following up within appropriate timeframes.
- Coding inaccuracies. Using the wrong ICD-10 or CPT code — or unbundling codes incorrectly — leads to denials that eat up weeks of extra work to resolve.
- Late claim submissions. Every payer has a timely filing deadline. Missing it means automatic denial — and you may never recover that revenue.
- Inadequate denial management. Denials that aren’t appealed promptly and strategically are revenue walking out the door.
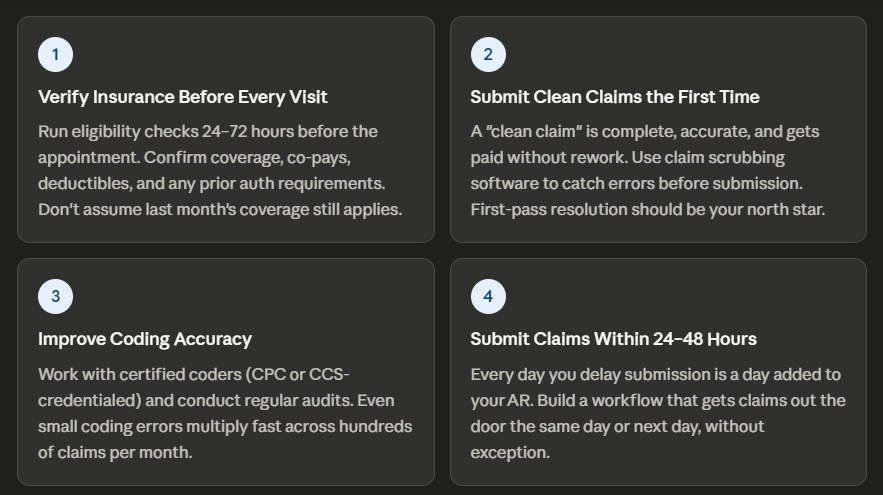
Proven Strategies to Reduce AR Days in Healthcare
Here’s the practical part. These aren’t vague suggestions — these are the actual steps that high-performing practices use to keep their AR days low and their cash flow healthy.
Best Practices for Faster Payments and Better Cash Flow
Beyond the basics, these operational habits separate practices that struggle with AR from those that consistently improve cash flow in healthcare:
- Hold weekly AR review meetings. Even a 20-minute weekly huddle where your billing team reviews the aging report can catch problems before they snowball.
- Invest in ongoing staff training. Payer policies change. Coding updates roll out annually. A team that stays current makes fewer errors and recovers more revenue.
- Use analytics and dashboards proactively. Don’t just pull reports when things go wrong. Build a habit of reviewing your denial dashboard and aging buckets every week.
- Offer patient-friendly payment options. More than 60% of patients say they’d pay their balance faster if offered payment plans or online options. Patient collections are part of AR too.
- Communicate clearly about financial responsibility. Patients who understand their cost-sharing obligations before their visit are far more likely to pay promptly after it
How Outsourcing Billing Helps Reduce AR Days
Here’s a question worth asking honestly: does your current in-house billing team have the bandwidth, the tools, and the expertise to stay on top of every claim, every denial, and every payer policy update — all while supporting your clinical staff?
For many practices, the answer is no. And that’s not a failure — it’s just reality. Billing is an entire specialty in itself.
When you outsource your revenue cycle to a dedicated medical billing company, you get:
- Specialized billing expertise. Dedicated billers who know payer-specific rules, timely filing deadlines, and denial appeal strategies for your specialty.
- Faster claim turnaround. Outsourced billing teams are built for speed and accuracy — claims go out same-day, follow-ups happen on schedule.
- Lower denial rates. When billing is done by trained specialists using the right tools, fewer claims go out wrong — and fewer come back as denials.
- Better visibility into your revenue cycle. A good billing partner gives you real-time dashboards and monthly reporting so you always know exactly where your money is.
- More time for patient care. Your team stops chasing insurance companies and starts focusing on what they were trained to do.
At Malakos Healthcare Solutions, we specialize in helping US medical practices reduce AR days, recover denied revenue, and build cleaner, more efficient billing processes — without the overhead of an in-house billing department.
Conclusion: Start Reducing AR Days Today
High AR days don’t just hurt your bottom line — they drain your team’s energy, limit your practice’s growth, and make it harder to deliver great care when financial stress is always lurking in the background.
The good news? This is a fixable problem. With the right processes, the right tools, and the right team, most practices can meaningfully reduce their AR days within 60–90 days of making targeted improvements.
References & External Resources
CMS.gov — Clean Claims and Timely Filing Guidelines
HHS.gov — HIPAA Transactions and Code Sets (Billing Standards)
NIH / PubMed — Administrative Costs and Inefficiencies in US Healthcare Billing
By Malakos Healthcare Solutions Revenue Cycle Management April 2026







2 Comments
First Pass Claim Rate: How to Improve It in Billing - Malakos Healthcare Solutions
[…] Outsourcing Medical Billing Improves First Pass Claim […]
“Prior Authorization in Medical Billing: How to Avoid Delays 2026” - Malakos Healthcare Solutions
[…] Why Outsourcing Prior Authorization Helps […]